The Double-Sided Nature of Big Data in Health Care

When data assets are transformed into data insights, everyone wins — leading to lower health care costs, healthier patients, improved consumer and staff satisfaction and greater understanding and transparency in processes for all.
Big data’s actionable insights have the ability to create a culture of meaningful health care, yet there are many roadblocks to overcome on the way there. Provider organizers must take a closer look at how they collect, store, analyze and present data to patients, staff and business partners to avoid a data mess without any beneficial or relevant insights.
What is the most meaningful way to offer these insights? Here are the benefits and challenges providers face when it comes to these big data issues, with approaches to resolve these obstacles to cultivate a culture of meaningful health care and success in the long haul.
The Larger Impact of Data Collection
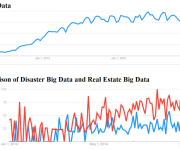
The gathering of population data typically drives big data statistics for medical research, yet medical care data is driven by information gathered on an individual level. Individual-level statistics must be made available in a way that is meaningful and accessible for all, particularly non-scientists.
Algorithms and interfaces must be created as graphical representations that offer an intuitive understanding, allowing people to make sense of the details of big data without needing irrelevant commands to access the information.
Information technology and big data have the potential to transform medicine. For example, medicine is becoming more elegant and precise to smaller groups and individuals, tailoring diagnoses and tests built on their unique genetic makeups with respect for personal autonomy through ethical analysis.
Artificial intelligence has the potential to fill in the gaps of data humans cannot collect and process in a timely manner. Predictive modeling optimizes how health care resources will be allocated to the community to meet the greatest needs.
Data Collection, Storage and Analysis Must Be Transparent
Data collection quickly becomes expensive, and providers must weigh the risks with the potential rewards of insightful innovation. In people’s everyday lives, there is a greater call for transparency on where and how medicines are sourced and why particular choices are made.
Health care providers should update IT infrastructures however possible. Unfortunately, electronic health care records are constructed to optimize how providers bill, not how they provide care. One of the biggest challenges providers face is streamlining data across infrastructures to work together and provide meaningful analysis.
Providers must ask themselves: “Are we delivering the right data?” Ideally, big data will be able to express the state of a patient in a meaningful way that shows more than what they owe, which is also a major source of frustration for patients. The variability of procedural total costs differ, sometimes drastically, and to fill the gap, many employers collaborate with third-party administrators or vendors to supply more transparent health care cost information to their staff.
Those in the front lines of health care cannot gain relevant information from patient claims, which are often months or even years outdated. Claims address billing, not vital clinical details that detail the care process. Here is an example of an opportunity to provide relevant and meaningful information that solves many frustrations for patients and clinicians.
Helpful Big Data Streamlining Solutions
Clinicians are understandably particular about operating room and clinic cleanliness, but what about the integrity of their data?
Most data cleaning takes place manually, but some third-party IT vendors provide automated tools that use logic rules to scrub data: comparing, contrasting and correcting large datasets. Increasingly, these tools are becoming more precise and sophisticated, ensuring accuracy and cleanliness in data collection.
One of the most powerful open-source data analysis platforms for big data is Hadoop. Originally developed to aggregate web search indexes and other routine functions, Hadoop has the potential to process large data amounts as an organizer and analyzer tool. Multiple vendors, such as Cloudera and AWS, distribute open-source software, and propriety options such as HBase and Cassandra are also available as database components.
Such cloud-based programs and open-source platforms help keep big data costs low for providers. However, many of these open-source tools need programming, and the issues of privacy and security must be addressed. The payoff comes in meaningful data that may be used to develop case protocols and care protocols, while gaining greater insight into the delivery of health care operations.
According to a report by McKinsey, if U.S. health care providers used big data creatively to drive quality and efficiency, it could generate more than $300 billion in value in the public sector. Two-thirds of this could reduce U.S. health care spending by roughly 8 percent. A retailer that used big data to its maximum potential could, in theory, boost its operating margin by more than 60 percent.
Using big data to revolutionize the health care industry is not about tossing technology at the problem and offering various numbers to consumers and relevant parties. Improving and integrating datasets can also benefit how medical researchers gather and use population data. For example, it will be easier to see which patients have missed vital screenings or are taking numerous medications with contraindications.
Big data has the potential to transform medicine in a meaningful way, and to do so, data must be shared and displayed in a way that is intuitive and meaningful for all, ultimately transforming confusion into understanding and knowledge that empowers, to the benefit of patients, staff and providers.
The post is by Nathan Sykes, a business writer with a passion for tech and IT. To see more posts by Nathan, you can read his blog, Finding An Outlet, or follow him on Twitter.